🔴 Website 👉 https://u-s-news.com/
Telegram 👉 https://t.me/usnewscom_channel
“Can someone bring an ultrasound into triage 3?”
On labor and delivery, these words, especially when spoken gravely by a senior nurse, are a code: I cannot find the heartbeat. I am worried that there isn’t one.
The attending physician and I each take a pass with the ultrasound, pausing on a heart that should be beating, hoping beyond hope to be mistaken. But then we must tell her.
There is no sound on Earth like a mother’s scream for her baby who will never get to breathe their first breath. Every mother begs for answers, wanting to know: Why? Why my baby? What did I do wrong? Why did this happen? Why, why, why, why, why?
This mother, 36 weeks pregnant, also sobbed, “What if I’d gone to the clinic?”
She was considered high-risk, and recommended for twice-weekly fetal monitoring. She attended those appointments faithfully — until reports of ICE activity in her hometown in North Carolina.
That week, she stopped leaving her house. She ordered groceries online, called out from work and kept her older child home from day care. Out of fear for her family’s safety, she also stopped coming to her obstetric appointments.
We will never know if fetal monitoring could have changed the outcome for her baby. Even with our best tests — autopsy, genetic analysis, lab work — we only identify the cause of fetal demise about half of the time. What I do know is that she will always wonder, as does every mother who has suffered pregnancy loss, what could I have done differently?
It is too much of a burden to also carry: What if I had gone to that appointment?
This patient is not alone. In a recent poll of more than 500 pregnant people, 20% of the respondents said that ICE activity has deterred them from accessing prenatal care.
“Patients are presenting in labor who have not had prenatal care since the raids in November. Our maternal-fetal medicine colleagues indicate record no-show rates to ultrasound appointments.”
We know that this will have devastating consequences. Throughout pregnancy, and especially in the third trimester, pregnant patients are monitored closely for conditions that could place them or their babies at risk. This includes blood pressure monitoring for preeclampsia, checking for signs or symptoms of early labor and, like this patient, fetal monitoring to detect increased risk of stillbirth. Missing these visits means missed opportunities to intervene before conditions become fatal to the baby, the mom or both.
A study of over 25,000,000 birth outcomes found that the risk of prematurity, stillbirth and infant death was not just increased with lack of prenatal care, but the relationship was linear: The less prenatal care received, the more likely babies were to die, either in utero or in the first year of life.
These consequences are not limited to obstetrics. Providers of all specialties in targeted cities are sounding the alarm that patients with chronic conditions are missing appointments that will affect their long-term health.
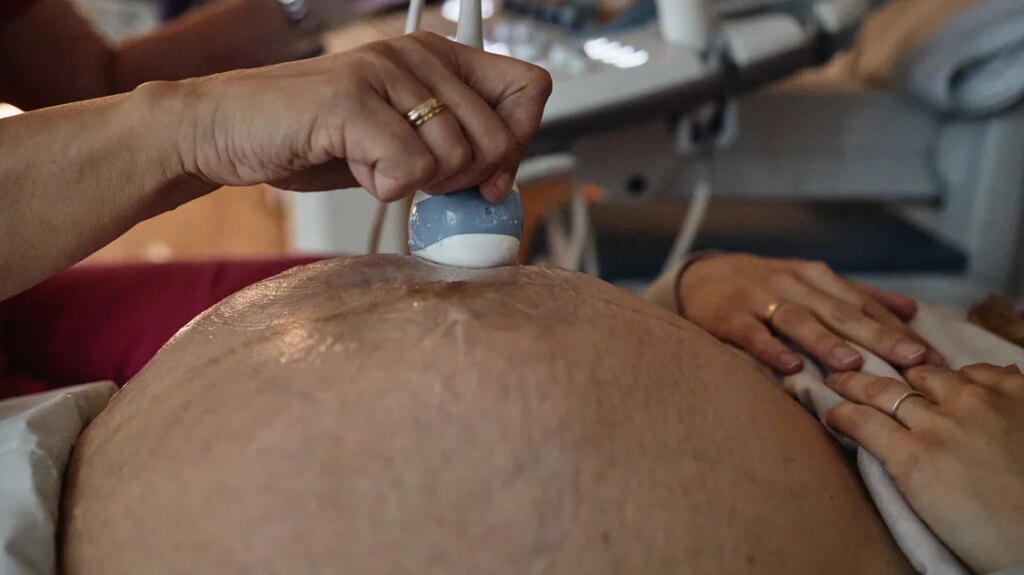
Operation “Charlotte’s Web”— a Border Patrol operation focused on the Charlotte area and neighboring cities — lasted less than a week, with long-lasting effects on the community. Months later, patients are presenting in labor who have not had prenatal care since the raids in November. Our maternal-fetal medicine colleagues indicate record no-show rates to ultrasound appointments — typically a highlight of prenatal care and a coveted appointment for most pregnant patients.
ICE has terrorized our communities and forced our neighbors — and my patients — into impossible choices: Risk being separated from your 3-year-old by attending a clinic appointment for your unborn child, or stay home and risk a pregnancy complication, or even the loss of your baby?
No one should be forced to make that decision.
Immigration enforcement policies are fracturing families, eroding trust in public institutions and creating a climate of fear that ripples through every aspect of life — work, school and even the most basic human need: seeking health care.
As a physician, I see the human cost every day. It is time to speak out — not only for our patients’ health but for their dignity, their families and their right to live without fear.
Do you have a compelling personal story you’d like to see published on HuffPost? Find out what we’re looking for here and send us a pitch at pitch@huffpost.com.